

 |

|
|
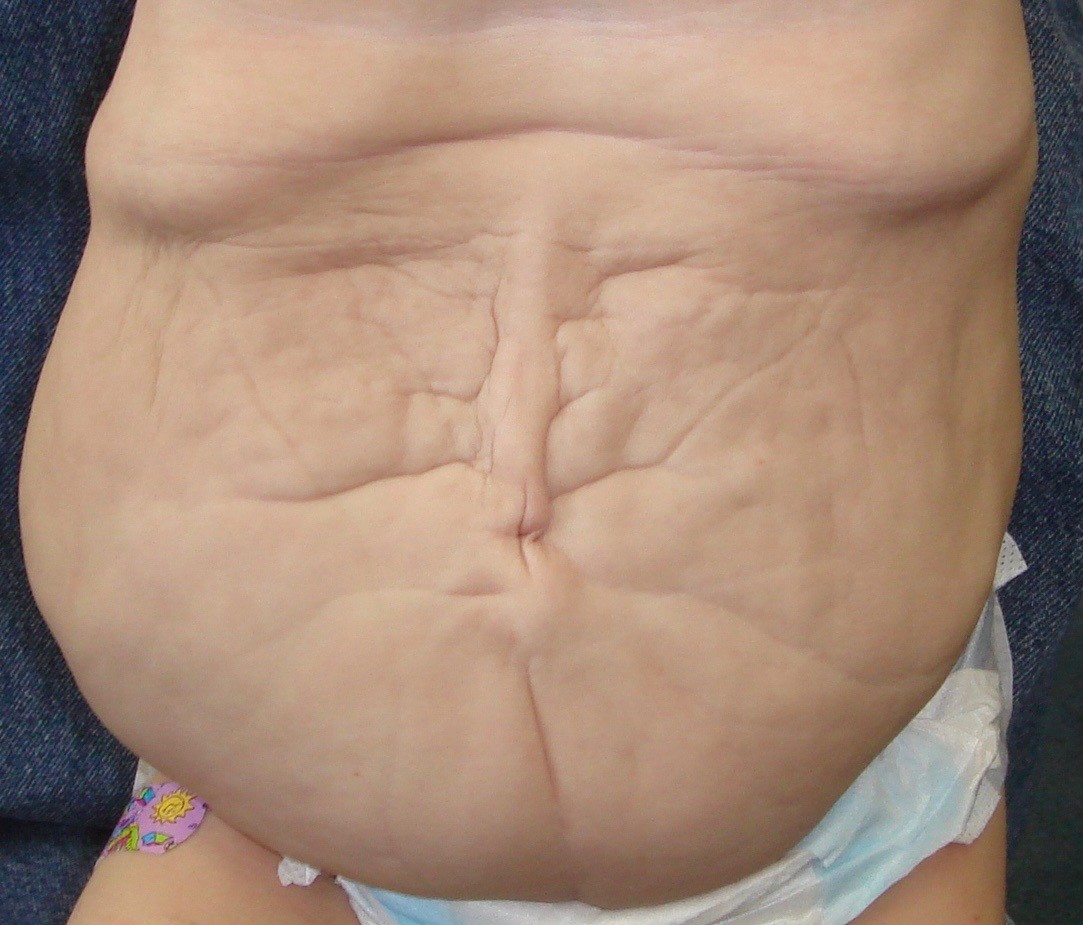 |
Prune Belly Syndrome Prune Belly Syndrome (also called PBS, or Eagle-Barrett syndrome) is a rare condition where babies are born without any muscles in the stomach region. The diagnosis is evident right at birth: without stomach muscles, the skin overlying the stomach becomes stretched out and wrinkled. Not only is the appearance of the stomach impacted, there are also some significant functional issues associated with this condition. Without stomach muscles, children are not able to increase the pressure inside their abdomens, making it harder to completely empty their bladder, which can lead to the development of a larger stretched-out bladder. If left untreated, the ureters (tubes between the kidneys and bladder) and the kidneys can swell, eventually producing a loss of kidney function. The lack of stomach muscles also makes it harder for children to cough deeply, resulting in more respiratory illnesses and even pneumonia. Many children may also face problems with constipation caused by the inability to “bear down.” Lastly, the loss of muscles, and core strength, on the front side of the spine makes it harder to maintain trunk control, limiting some movements. Prune Belly Syndrome primarily affects boys, although some girls can also be born with this condition. In addition to the loss of stomach muscles, boys will also have cryptorchidism, which means “hidden testicles.” Normally the testicles form inside the abdomen and then descend into the scrotum sometime before birth. With Prune Belly Syndrome, this descent does not take place leaving the testicles inside the abdomen. Treatment One of the earliest things to assess for any child born with Prune Belly Syndrome is kidney function. Your urologist will typically schedule tests to see how well your child’s bladder is emptying. If blood tests suggest that there is some reduced kidney function, a nephrologist, or kidney specialist, may also be consulted to follow your child. The second area to address is the cryptorchidism. It is important for urologists to bring the testicles down into the scrotum, in order to improve the ability to monitor for the low but significant risk for testicular cancer. Often, the operation to bring the testicles down into the scrotum, which is called an orchidopexy, requires making an incision in the stomach to enable the urologist to find the testicles, in order to bring them down into the scrotum. It is generally recommended that this operation be performed before puberty, although the precise timing for this procedure may vary, depending on your doctor. This operation can be performed as an isolated procedure, or at larger centers is often combined with another procedure called an abdominoplasty, which tightens up the stomach by removing some the excess skin. There are two types of abdominoplasties for children with PBS. The first, and most commonly performed, is the standard abdominoplasty. This is a static procedure, meaning there is no movement of the stomach wall after the surgery is completed. The second type of abdominoplasty is a newer procedure called a dynamic abdominoplasty, meaning there is some movement of the stomach following the procedure. During the standard abdominoplasty operation, the surgeon separates the top skin layer from the deeper fascial layer (which is the strongest layer in the stomach), in order to tighten this layer up. After the fascia has been tightened, the excess skin is removed and the incision is closed. This operation helps to improve the appearance of the stomach and may offer some additional support. At our center in Dallas, we helped to develop and refine the dynamic abdominoplasty procedure. We believe this operation provides children with better function afterwards than is possible with the standard abdominoplasty. This newer procedure begins by performing a traditional static abdominoplasty with a tightening up the fascia. However, before the excess skin is removed, an additional step is added. This step entails releasing the attachment to the knee cap of one of the four muscles on the front of each thigh so it can be moved to the stomach. These muscles are then tunneled under the groin area into the stomach region on both sides and are then attached to the deep fascia somewhere below the rib cage. By taking a working muscle from the thigh and moving it into the stomach, this allows children to increase pressure inside their stomachs. Increasing pressure inside the abdomen is necessary to deeply cough, empty the bladder, and to facilitate bowel function. In addition, these transposed muscles bring muscular forces to the front of the spine to balance those behind the spine, which has the potential to improve core strength and trunk control. The long-term effects of providing some muscles in front of the spine to balance the already existing muscles behind the spine, with respect to preventing back pain later in life, has yet to be studied. We recommend delaying the dynamic abdominoplasty operation until after a child has reached at least 18-months of age. After that, there is no upper age limit. Following this operation, older children have reported immediately noticing improved trunk control, assisting them with the ability to bend forward and then straighten up again. We are aware of one study that has examined the side effects of taking one of the four muscles of the thigh. This study performed strength testing in both legs after patients had one muscle taken from just one side. Somewhat surprisingly, they found no significant differences in strength between the two sides. This is probably because the remaining three muscles on the operated side strengthened up to compensate for the loss of that single muscle. Based on this study, it seems that children are not giving up any obviously longer-term measurable functional loss in order to gain functioning muscles in their stomachs. It is always a good idea to seek additional opinions before beginning any treatment. Many families choose to seek care for their child further from home in order to get what they believe is the best care for their child. Not only do surgeons differ on how they perform operations, they also can differ on communication styles and treatment philosophies. Visiting more than one center will help families chose a team that is the “right fit.” Jeffrey A. Fearon, MD |