| |
Cleft Lip and Palate:
Overview:
Cleft Lip and Palate
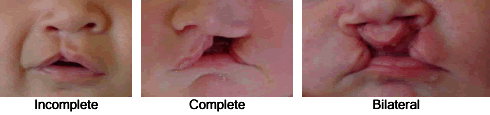
Clefts are relatively common, occurring somewhere between 1 in 500, to 1 in 2000 births, depending on the culture of the parents. For example, the incidence is lower in families coming from Africa but much higher in families coming from Asia. Children can be born with just a cleft of the lip, a cleft of the palate (roof of the mouth), or both a cleft lip and palate. The cleft lip can be incomplete, complete, or bilateral (see Figure Cleft Types).
What causes a cleft?
Clefts of the lip and palate are some of the most common birth defects in newborns. A cleft does not occur because of any one thing in particular that a mother might have done or not done during her pregnancy. Interestingly, almost a third of all babies born with a cleft will have some relative on either parent’s side that also was born with a cleft. This raises questions about the role that genes might play in cleft lip and palate. In fact, a number of genes have been discovered that are associated with clefts. However, it is currently believed that these genes do not cause the cleft; they appear to just make them more likely to occur. A number of different drugs (alcohol, cigarettes, some seizure medications, vitamin A derivatives) have also been shown to make clefts more likely and there is some evidence to suggest that taking prenatal vitamins before conception may lower the chance of having a child with a cleft. However, it is most likely that a number of factors must come together for a cleft to occur. Once a family has a child with a cleft lip and palate, the chances of having a second child with a cleft is about 4%, so many families find it helpful to meet with a geneticist to further discuss these issues.
How are clefts treated?
The treatment that a child born with a cleft might need depends upon whether or not there is just an isolated cleft lip, an isolated cleft palate, or both together. If a child is born with only a cleft palate, then an evaluation with a geneticist becomes even more important, to test for certain conditions such as: Pierre Robin Sequence, velocardiofacial, DiGeorge, Stickler, among others. There are a number of different ways to repair clefts, and surgeons will vary on when it is the best time to do this and which technique they prefer. This section will first review some of the more commonly recommended treatments and then will discuss what we recommend for our patients at the Craniofacial Center in Dallas.
Step 1. Feeding and the initial evaluation.
Children born with a cleft palate cannot create enough suction while feeding and therefore will have difficulty getting sufficient milk to grow normally. This inability to create enough suction comes from the opening in the roof of the mouth, which allows air to come in through the nose when the baby is trying to create enough suction to swallow. Less suction means less volume so the baby must work harder to get any milk at all, and whatever is swallowed is usually mixed with a lot of air that can cause colic. If mothers attempt to breast feed their baby, or use a regular bottle and nipple, they will find that after about 30 minutes their baby will get tired of trying to get enough milk and will fall asleep. Then, 60-90 minutes later their baby will wake up again, crying and hungry. The result of this cycle is that the baby does not gain enough weight to grow normally and the parents become exhausted. Therefore, shortly after birth a feeding specialist (typically a speech pathologist or occupational therapist) is called in to help. There are a few different ways to feed a baby with a cleft palate and often it takes trying more than one way to find out which is best for each child. One method is to enlarge the hole in an extra soft nipple; so when baby compresses the nipple, milk will stream out by gravity. It usually does not take very long for an infant to learn how to control the amount of milk (breast or formula) that will flow out of the bottle by gravity. Another commonly used method is to feed the baby with a squeeze bottle called a Haberman feeder, where either the baby or the parent can squeeze a little milk into the mouth before each swallow. Whatever technique works the best, it is important that a baby gets enough milk per feeding to be able to grow normally.
2. Presurgical orthopedics.
This term refers to any technique that is used before surgery to move both sides of the cleft in order to narrow or better position each side, with the goal of making the eventual repair easier. There are a number of different types of presurgical orthopedics that might be recommended. The most simple of these is a specialized elastic tape, which is stretched across the cleft on top of the cheek skin in order to slowly bring the two sides of the cleft lip closer together. Although this requires keeping tape across a baby’s lip, it can be surprising how just over the course of a few weeks the two sides will come so much closer together. For babies born with bilateral clefts, this taping can help better position the central part of the lip, called the prolabium, which tends to stick out too far forward (see Figure, Prominent Prolabium)
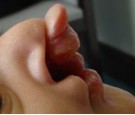 Prominent Prolabium Prominent Prolabium
Another type of presurgical orthopedics that might be recommended is called NAM, which is short for nasoalveolar molding. This process entails creating a splint that is worn inside the baby’s mouth, with posts coming off the top of the splint that push up the nose from the inside. NAM requires weekly visits to an orthodontist, who needs to continually reshape the plate inside the mouth, as well as to lengthen the posts pushing up the nose, in order to accommodate the rapid growth of the baby. This technique is less commonly performed, partly because of the frequent adjustments that are required; nevertheless, there are a few centers that are very enthusiastic about using NAM.
3. The lip repair.
The traditional timing for repairing a cleft lip is sometime around 12 weeks of age. Parents may hear about the “rule of 10’s,” which means that the repair should wait until the baby is 10 weeks old, the hemoglobin (blood level) is over 10, and the baby weighs at least 10 pounds. However, some surgeons might recommend even earlier surgery to perform what is called a lip adhesion. This procedure is often done as early 6 weeks of age. The lip adhesion doesn’t completely repair the cleft lip, but instead just pulls the two sides of the lip together, with the intention of making the final repair at 12 weeks of age easier to perform. Today, lip adhesions are less commonly done, although some surgeons might feel that an adhesion is needed for particularly wide, or a bilateral cleft. The majority of craniofacial surgeons will recommend a cleft lip repair sometime after 3 months of age. The lip is typically closed using either dissolving sutures or permanent stitches that must be taken out 5 days later. Babies spend at least one night in the hospital before being discharged home with arm restraints called “no-no’s,” made of either cloth or plastic, which are wrapped around the elbows after surgery. These arm restraints are intended to prevent babies from putting their fingers inside their mouths. Some doctors might also recommend that babies not be fed with a nipple after the surgery, instead using either a cup or a syringe technique. There are also some surgeons who might wish to simultaneously close the back half of a cleft palate at the same time as doing the lip repair; then about 9 months later, close the front half with a second operation.
4. The palate repair.
The majority of cleft surgeons will recommend repairing the cleft palate (both hard and soft) as a single operation sometime between 9 and 18 months of age. There are some studies that suggest doing the palate repair at an earlier age has advantages, but then there are other studies that suggest that doing the repair later is better. It is believed that the earlier the repair the better the speech outcomes, but the later the repair the better the growth of the upper jaw. The theory is that if the upper jaw can grow better, there is less of a likelihood that a child might need to undergo jaw surgery as a teenager. Not only do surgeons vary on when they recommend fixing the palate, they also vary on how it is repaired. There are a number of slightly different ways to close a cleft palate, but they all share in common moving either side of the cleft together so that the two halves meet in the midline. So, no tissue needs to be taken from somewhere else to fill in the cleft space. After the palate repair, children will spend at least one night in the hospital before going home. Most children are kept in “no-no’s and surgeons will vary on how a child is permitted to feed after the operation. Typically, children are not allowed to use a nipple after surgery.
5. The Ears
Children born with a cleft palate are more likely to develop fluid behind the eardrums, a condition called serous otitis media. This is because the muscles that normally open up the Eustachian tube are out of position, preventing the tube from opening in a normal way. Therefore, fluid builds up in the inner ear making it hard for children to hear clearly. At the current time, most otolaryngologists (ENT’s) recommend putting in ear tubes for any child with a cleft palate who has fluid behind the eardrums. Cleft lip and palate centers will coordinate the placement of ear tubes with other operations, such as the repair of the lip or the palate, in order to reduce the total number of anesthetics and operations a child will need. Long-term hearing loss can occur in children with clefts, especially if they have had multiple untreated ear infections.
6. Speech
Children who have undergone cleft palate repairs are more likely to have trouble speaking normally. If babies have not had tubes placed, or replaced when needed, speech may be delayed. The most common problem with speech after a cleft palate repair is nasal air emission. When we talk, the space between the back edge of the palate and the very back of the throat will open and close depending upon the sound that we are trying to make. In general, for vowel sounds this space is open and for consonants it is closed. Often, children born with a cleft palate will either have a short palate from front to back, which makes the space behind the palate bigger and harder to close. Or, they may have a palate that does not move as well. This problem with speech is called velopharyngeal incompetence, or sometimes just referred to as VPI. There is currently some controversy as to whether or not speech therapy alone can improve nasal air emission. When children are unable to make certain sounds because they cannot close off the back of the palate, they will learn other ways of faking these sounds (which are called substitutions). If these substitutions are not corrected early, they can be very difficult to unlearn. Many experienced speech pathologists believe that the greatest benefit from speech therapy is the ability to correct the learned errors associated with the inability to make certain sounds in a normal way, but that improving VPI is not always possible with therapy alone. In general, it is always a good idea to try speech therapy before thinking about doing another operation. However, for those children who just don’t seem to be improving with speech therapy, there are additional operations on the palate that can be done that can significantly improve speech, such as: a posterior pharyngeal flap (PPF or P-flap), a sphincter pharyngoplasty, and a Furlow (4-flap palatoplasty). When needed, these operations are usually done before age 6. There are pros and cons to each of these procedures and surgeons must select the right procedure for each child. Finally, it is suggested that children with cleft palates never get their adenoids removed because this can either cause, or worsen VPI.
7. Revision of the lip and nose repairs.
As children approach school age, surgeons may recommend one or more operations to further improve the appearance of the nose or upper lip, depending upon how well the results of the primary repair turned out. These operations are almost always performed as an outpatient and do not require overnight stays in the hospital. Some children may undergo 3 or 4 of these types of procedures during their growth years, depending on the surgeon.
8. Alveolar bone grafting.
Although babies born with cleft palates most often undergo closure of their clefts around a year of age, these operations usually do not close the entire cleft. Typically, a small gap is left in the front just underneath the upper lip, along the gum line. Why is this left open? It turns out that studies show that if you leave the cleft open in the gum line (also called the alveolus), the upper jaw may have slightly better growth than if it were closed at an early age. The hope is that this additional growth might lessen the chance that a child would subsequently require upper jaw surgery in teenage years. Most cleft teams recommend the alveolus be closed sometime between the ages of 7 and 9 years. For children treated at a cleft center, the team orthodontist is usually the one that determines the best timing for this closure. Frequently, the orthodontist will have placed a palatal expander prior to this surgery, in order to widen the arch of the upper jaw. During the operation, the alveolar cleft is filled with bone taken from near the child’s hip, which is covered using soft tissue coming from the adjacent gums. This bone helps the eruption of one of the permanent teeth called the canine tooth, but it also strengthens the arch of the upper jaw and provides some support for the base of the nose. Following this operation most children spend one or two nights in the hospital. A few surgeons might recommend placing a substance called BMP (bone morphogenic protein) in the cleft instead of using the child’s own bone. This substance causes the body fill the cleft with bone and has the advantage of not having to take bone from elsewhere (parents cannot donate bone to their children). However, a number of potential complications have been reported with the use of BMP in growing children, which has kept the FDA from approving its use for treating alveolar clefts in children.
8. Jaw Surgery.
Studies suggest that about 25% of all children born with a cleft lip and palate will require jaw surgery (called a Le Fort I) when they reach teenage years. Most often, this means simply moving the upper jaw forward, but sometimes it is necessary to also widen the upper jaw at the same time. This surgery can bring the child two benefits: it can significantly improve appearance and it also brings the teeth together into a normal relationship to improve the mechanics of chewing. Advancing the upper jaw can also increase the clarity of speech, by making more room for the tongue placement behind the upper teeth. Before the jaw surgery can be performed, it usually takes the orthodontist somewhere between 18 months and two years to align the arches of the teeth. During this process it may be recommended that some teeth be pulled, as well. For those children whose midface is set back further than average, a technique called distraction may be recommended, which can slowly bring the upper jaw forward much further than with a simple jaw surgery.
How clefts are treated at the Craniofacial Center
First and foremost, it is our goal to reduce the total number of operations that most children with a cleft lip and palate undergo. Our treatment philosophy is that it is best for children to grow up thinking of themselves as being normal person and not someone with a cleft lip and palate. We believe that the best way to achieve this is by minimizing the total number of medical visits and operations. As a general rule of thumb, less surgery is better than more surgery. Here is a brief overview of a typical treatment plan at our center in Dallas:
1. Initial treatment.
All babies born with a cleft palate undergo an initial evaluation with our feeding specialist to ensure that they are not having any problems growing and gaining weight. Once we are confident that babies are feeding well, nothing further is usually recommended until the lip repair. We recognize that some centers want to get babies started on nasoalveolar molding (NAM) right away, but we do not recommend this treatment for our patients. The reasons for this are complicated, but the bottom line is that we do not believe that it is possible in teenage years to tell the difference between children who underwent this labor-intensive treatment, from those who did not. We also do not recommend cleft lip adhesions, which we believe adds an additional operation that does not produce a measurable benefit to the child over the long-term. However, for some children with bilateral cleft lips, we may recommend conservative taping leading up to the repair. Prior to performing any operation (i.e. the lip repair or the palate repair), babies are evaluated by an ENT to see if tubes need to be placed in the ears at the same time, because we do not want children undergoing separate operations.
2. The lip repair.
There have been some relatively new studies that have raised questions about the effects of anesthesia on the developing brain (see the SmartTots website). Based on these concerns, we now delay the primary lip repair until over 6 months of age. Unlike most other teams, at our center this operation is done as a day surgery meaning that there is no need to spend the night in the hospital. During surgery the top skin layer of the upper lip is closed with a medical grade glue, instead of using stitches (see Figures below). We were the first to describe this special technique for closing clefts and we are convinced that this type of closure results in a much better scar than when skin stitches are used (see reference #32). During the lip repair, the nose is also rebalanced using a technique that minimizes internal scarring. After the operation babies are allowed to feed with a nipple, exactly the same way as they did prior to the operation, without any restrictions. We also do not require that babies wear “no-no’s,” which we believe only frustrate children without adding any benefit whatsoever.
3. Fixing the palate and speech.
We recommend repairing the palate sometime between 11 and 15 months of age and during this operation both the hard and soft palate are closed at the same time. Following this procedure, no restrictions are made on how the baby eats and once again for this operation as well, we do not use “no-no’s.” At our center, this is the only night that families typically need to spend in the hospital for at least the first 7 or 8 years of life. Following the palate repair children are followed by our team speech pathologist (and dentist, if necessary) to monitor the quality of their speech. Speech therapy is often recommended leading up to grade school. If children do require additional operations on the palate (about 20% need further palatal lengthening), we are most likely to recommend a 4-flap palatoplasty because we think that this operation is the least likely to produce subsequent problems with breathing through the nose. However, we also believe that every operation needs to be tailored to the unique needs of each child, so on occasion other procedures might be discussed.
4. Additional operations on the lip and nose.
While many centers routinely recommend “touch up” operations on the lip and nose, we have noticed that most children do not give their lip scars a second thought until they are older. So, following the philosophy: “ain’t broke, don’t fix,” any revisions of the nose or lip are left up entirely to the parents and children. We have noted that earlier operations are more likely to need to be repeated later and that the longer you wait to make a revision, the less likely that future operations need to be performed. So by waiting until families are convinced that children are ready for such surgery we believe that we can eliminate operations for the child, reducing the total number over a lifetime.
5. Alveolar bone grafting.
At our center, we only recommend using the child’s own bone for filling in the alveolar cleft. Our team orthodontist determines the timing for the operation. At the end of the operation, we insert a small tube called a pain pump, into the donor site where the bone was taken from (usually the right iliac crest, which is next to the hip). For 5 days after the operation, a small amount of numbing medicine is delivered to the donor site, which we have noted has significantly reduced soreness. This treatment has been so effective that we have found that some children do not even have to spend one night in the hospital after surgery and are ready to go home on the same day as the operation. We do leave this decision up to the child and parent, recognizing that each child heals in differently. However, most children are more comfortable and feel less threatened if they are sleeping in their own beds at home.
6. After the bone graft.
Once children have undergone alveolar bone grafting, there is the possibility that no further operations might be needed. We follow children through growth into teenage years (and even well into adulthood, when needed). Our team orthodontist and dentist closely follow children who live near to our center. For those who live further away, our orthodontist may supervise the care of a local orthodontist. While there is the possibility the jaw surgery may be required at the completion of growth, any subsequent revisions on the nose, lip, or even for speech, are performed only when the children and their parents believe that such procedures would be of significant benefit. Once again, we believe that the best treatment is one that allows children to grow up seeing themselves as the normal persons that they are, in part by minimizing the total number of operations they must undergo. Furthermore, another benefit of doing fewer operations is avoiding the “operated on” look. Fewer well-timed operations often produce a much better appearance.
There are well over 100 cleft lip and palate teams in North America, as listed by the American Cleft Palate - Craniofacial Association (www.acpa-cpf.org). In most urban areas, families will have more than one team available to them. We recommend that families get at least two different opinions before choosing the team that will care for their child. Some families may choose to seek care for their child further from home to get what they believe is the best care for their child. Not only do surgeons differ on how they do the operation, they differ on communication skills and treatment styles. Visiting more than one team will help families chose a team that is the “right fit” for them.
Jeffrey A. Fearon, MD
Cranio700@gmail.com
972-566-6464
|
|



